PRIORITIES
PARTNERS IN RESTORATIVE CARE
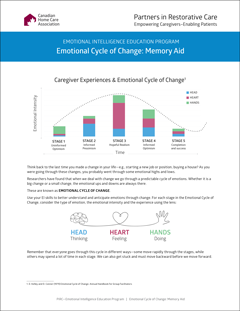
- How can health care providers empower patients and their caregivers as they deal with the emotional cycles of change throughout their care journey?
- How can patients and caregivers develop the confidence and ability to be partners in their care journey?
- What do providers need to do differently to recognize, understand and respond to patients’ and caregivers’ needs?